Advanced imaging reveals pilot’s high risk for heart attack
When it comes to siblings, some childhood habits never end — like keeping score and comparing how you measure up. For 53-year-old Dave Powell, it possibly saved his life.
When one of Dave's brothers was instructed to have a cardiac CT by his family doctor, he found that he had a small amount of plaque in his coronary arteries. He then warned his siblings to get their calcium scores checked as well. Family history can increase a person's risk for coronary artery disease (CAD).
Calcium score testing
A calcium score test is a CT scan that reveals how much calcified plaque has built up in the arteries of the heart. A waxy, fatty substance, plaque interferes with blood flow and can lead to a heart attack.
Along with a test result of positive or negative, patients receive a number that correlates with their risk: 100 or less shows mild proof of CAD. Over 400 strongly indicates CAD and a heightened risk of heart attack. Alarmingly, Dave's sister scored 600, which prompted him to take immediate action.
Temporarily grounded
Dave's interest in finding out his risk for a heart attack wasn't just personal. He's a professional pilot who flies people on private charters.
"I told my doctor I needed to know I was safe to fly people around. It's a big responsibility," he said.
Dave had to convince his (now former) primary care physician to refer him to a cardiologist for a coronary calcium scan, but he prevailed. The test came back positive. His score: 1100.
"I was pretty scared," Dave admits.
Dave reported his results to the Federal Aviation Administration (FAA), per regulations, and was effectively grounded pending further testing. That's when Dave really had to advocate for himself.
His cardiologist (not affiliated with Main Line Health) didn't see a need for immediate testing and wanted to wait 6–8 months. He acquiesced when Dave insisted, and administered a stress test, which Dave passed.
The pilots' association to which he belongs recommended cardiac catheterization in order to get medical clearance to resume flying. Then Dave learned of another option.
HeartFlow 3D Imaging
For a patient like Dave who is asymptomatic, cardiac catheterization is an invasive choice. Discussing options with his Aviation Medical Examiner (AME), Dave learned he could have a cardiac computed tomography angiography (CCTA) as a next step, as long as it included HeartFlow.
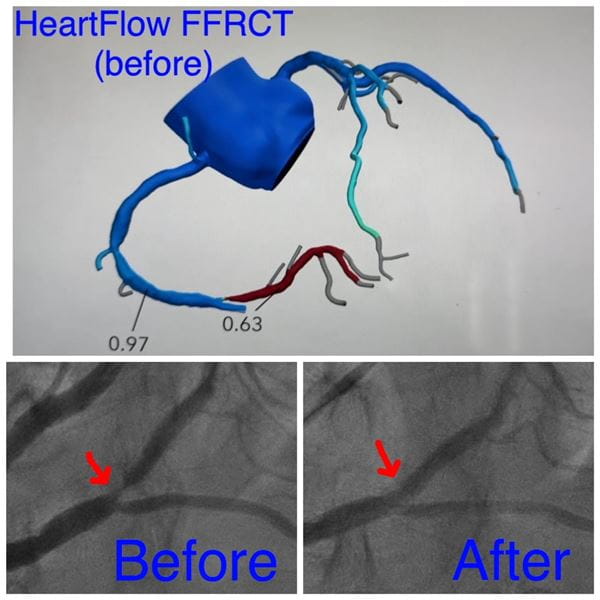
"My AME doctor contacted the company and asked who had that capability in the Philadelphia area. They answered: Main Line Health," Dave said.
Lankenau Heart Institute, part of Main Line Health, is the first in the region to offer this advanced diagnostic tool. Dave had his FFRct in early March 2023 at Riddle Hospital, part of Main Line Health. The results came back positive, revealing a vessel that was more than 90% blocked.
Cardiac catheterization and a stent
Dave contacted Main Line Health and scheduled an appointment for a consult with interventional cardiologist, Neerav Sheth, MD. Immediately, he knew he was in good hands.
"Dr. Sheth was a great listener with a really good bedside manner. He was familiar with HeartFlow and how it worked," Dave said.
Dave's next step was a cardiac catheterization to confirm the blockage, open it and insert a stent.
"The CT with HeartFlow flagged a significant blockage on a large branch on the bottom of his heart. We did a catheterization and it was spot-on with the HeartFlow image," Dr. Sheth explained.
Dr. Sheth performed the procedure at Paoli Hospital, part of Main Line Health, and Dave went home the same day. Coincidentally, Paoli Hospital is where Dave's father underwent a triple heart bypass twenty years earlier. He's alive and well today.
Communication and self-advocacy
Dr. Sheth explained that when a patient is asymptomatic, like Dave, it doesn't mean early detection of heart disease isn't possible, but it does mean both doctor and patient need good communication.
"In David's case, because he was so active and so asymptomatic, I'm not surprised his stress test was normal," Dr. Sheth said. He pointed out that there are questions physicians can ask to dig deeper if a patient says they have no symptoms.
"If the patient is telling the doctor I feel fine, I exercise, it creates a false sense of security and the doctor may agree to wait and recheck numbers later. But once you dive into the risk factors and the patient's personal and family history, you can uncover some red flags. Once they're uncovered, we know what to do," he said.
In other words, if you ask the right questions and give the patient a frame of reference, you'll start to get a more complete picture. Dr. Sheth asks patients about chest pain, shortness of breath, exercise endurance, family history, even unexplained health problems not related to the heart. Calcium scores and cholesterol numbers also help inform a patient's need for further testing or intervention.
Dr. Sheth's best advice: "Talk to your doctor. Make sure you're asking the right questions and giving the right answers. And ask your family members about their medical history — a lot of families don't share medical information, which is unfortunate. Dave was really proactive in his case. Bottom line: take ownership of your life."
As for Dave, he looks forward to getting back in the air. His determination to get tested in light of his family history led to his successful treatment while he was still a candidate for minimally invasive measures. He said, "Frankly, if I didn't take proactive steps, I think I would have needed heart bypass surgery. My artery was right at the borderline where it could barely be stented. Another five years and who knows?"
If Dave were ever to need heart surgery down the road, he'd be in great hands. Lankenau Heart Institute has the leading minimally invasive robotic-assisted coronary artery bypass program in the country, with long-term outcomes that meet or exceed those in groundbreaking international clinical trials.
Next steps:
Learn more about Neerav Sheth, MD
Learn more about Lankenau Heart Institute
Learn more about HeartFlow
Want to get the latest health and wellness articles delivered right to your inbox?
Subscribe to the Well Ahead Newsletter.
 Content you want, delivered to your inbox
Content you want, delivered to your inbox
Want to get the latest health and wellness articles delivered right to your inbox?
Subscribe to the Well Ahead Newsletter.
