Clinical trial provides Ben a minimally invasive route to beating cancer
Ben Deitrich was not one of those who dread their 40th birthday. With frequent outdoor family activities like camping and hiking and a satisfying construction management career, life was going too well for anything other than a cheerful outlook.
"It was the summer of 2017," Ben says. "I was feeling fantastic and telling my wife, 'You know, I feel like a young man.' It was around that time that I really noticed something was wrong."
He started suffering sudden, debilitating bouts of diarrhea. The cause turned out to be rectal cancer.
His first thoughts centered on survival and seeing his young family grow. But he was also focused on the highest quality of life. For most patients in the United States, the focal point of the treatment plan is surgery with a large incision to remove part of the colon, leaving them with a permanent colostomy bag outside the body to collect waste. However, a clinical trial at Lankenau Medical Center offered Ben a minimally invasive option.
John Marks, MD recommended a transanal total mesorectal excision (taTME), also known as "bottoms up" surgery—a procedure that was developed at Lankenau. It removes rectal cancer without the need for abdominal incisions or a colostomy bag.
Ben decided, both physically and for his state of mind, that the least invasive option was the one for him. And he trusted the Main Line Health team was steering him in the right direction.
"I wanted to position myself for the best possible future outcome," Ben explains. "So for me, it made sense, and it was a good decision."
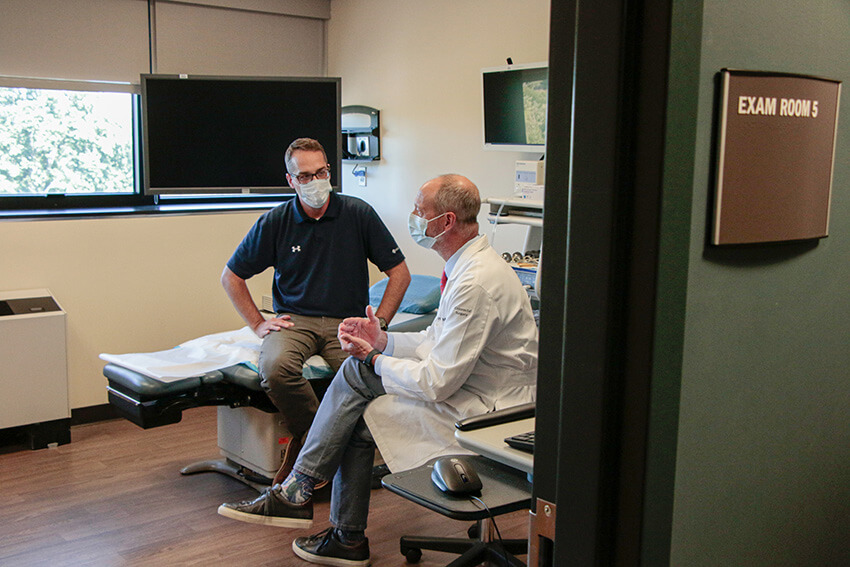
A pioneer in treating colorectal cancer
Many hospitals participating in the five-year multicenter clinical trial for taTME, which will provide the first standardized U.S. data on the procedure's safety and effectiveness, were just starting to gain experience with the procedure.
But Marks, who is chief of colorectal surgery at Main Line Health and a professor with the Lankenau Institute for Medical Research (the health system's research entity), had already performed it hundreds of times. Lankenau is among the top few centers nationally in taTME experience.
"I've been involved in teaching, performing and perfecting minimally invasive colon and rectal cancer for two decades now," Marks says. "The benefits are immense. You can see the difference between someone who had a big open operation and someone who didn't. You can see it by the way they walk, how much pain they're in, how uncomfortable they are, how quickly they get back to eating."
Historically, the rate of people needing a permanent colostomy for rectal cancer in America has been in the range of 40–60%.1 At Lankenau, the rate is 7–10%, and the rate of rectal cancer recurring is only about 2–3%. The national recurrence rate of around 7–10% has slowly been improving,2,3 partly through sharing of Marks' work and a national accreditation program in which he plays a leading role.
"Seeing the results five years down the line with such great outcomes is what's so rewarding about being a surgeon—and being a cancer surgeon, in particular," Marks says.
Too young for screening
Ben remembers the bewilderment he felt as he saw his primary care doctor for treatment in the summer of 2017. Why was he being sent to be tested for rectal cancer? He wasn't even near the recommended age of 50 to start being screened for it with a colonoscopy (since lowered to 45). But a colonoscopy and biopsy results confirmed the diagnosis that November.
Ben soon was referred to Marks. After consultation with a multidisciplinary team, Marks offered Ben the first spot in the clinical trial.
"I was thankful for some specialists within the Main Line Health network that recommended me to Dr. Marks' practice," Ben says. "Once I learned about his program and his track record and history of performing these procedures, I was fully convinced that this was the right place for me, and I was committed to following the path together with Dr. Marks."
A difficult road followed by recovery
Not fully comprehending what lie ahead but knowing it would be difficult, Ben did his best to enjoy a late autumn vacation to Walt Disney World with wife Marilu, daughter Eliza, who was 11 at the time, and son Evan, who was 9. Within a few days of their return, he began radiation and his first course of chemotherapy to shrink the tumor.
Ben coped with the challenge by leaning into his personality and professional training. In his construction management work, he focuses on short-term goals to complete complex building projects. He did the same with his cancer treatment plan.
"I knew it was going to be tough, but I didn't necessarily comprehend how tough the recovery from surgery combined with chemotherapy would be," he says. "I'm a very goal-oriented person. So I created checklists. And when I knocked off a round of radiation or chemo, I was like, 'That's one obstacle out of my way.'"
Ben underwent taTME in March 2018 and a follow-up procedure nine months afterward. In late 2019, about a year and a half after the initial procedure, he finally felt like himself again. The decision to participate in the clinical trial had paid off.
"Not being an expert in the field and having a young family, my wife and I were just trying to come to a consensus on the best course of action," Ben says. "I didn't want a treatment that would have a negative impact on me for the next 40 years of my life."
Adds Marks: "Ben did great with his procedure. Cancer is not for sissies. It's a hard road. Patients like Ben are really the warriors who fight the fight, and we're there to give them the best cancer care and support them."
To learn more about Lankenau Institute for Medical Research cancer clinical trials, call the cancer trials team at 484.476.8426 or email us at [email protected].
1 Steven D. Wexner and Christopher M. White, Improving Rectal Cancer Outcomes with the National Accreditation Program for Rectal Cancer, Clinics in Colon and Rectal Surgery 33, (2020): 318–324.
2 John H. Marks, Renee Huang, Dominique McKeever and Morgan Greenfield. "Outcomes in 132 Patients Following Laparoscopic Total Mesorectal Excision (TME) for Rectal Cancer with Greater Than 5-Year Follow-Up," Surgical Endoscopy 30, no. 1 (2016): 307–14.
3 James Fleshman, Megan E. Branda, et al., "Disease Free Survival and Local Recurrence for Laparoscopic Resection Compared to Open Resection of Stage II-III Rectal Cancer: Follow-Up Results of the ACOSOG Z6051 Randomized Controlled Trial," Annals of Surgery 269, no. 4 (2019): 589–595. doi:10.1097/SLA.0000000000003002.